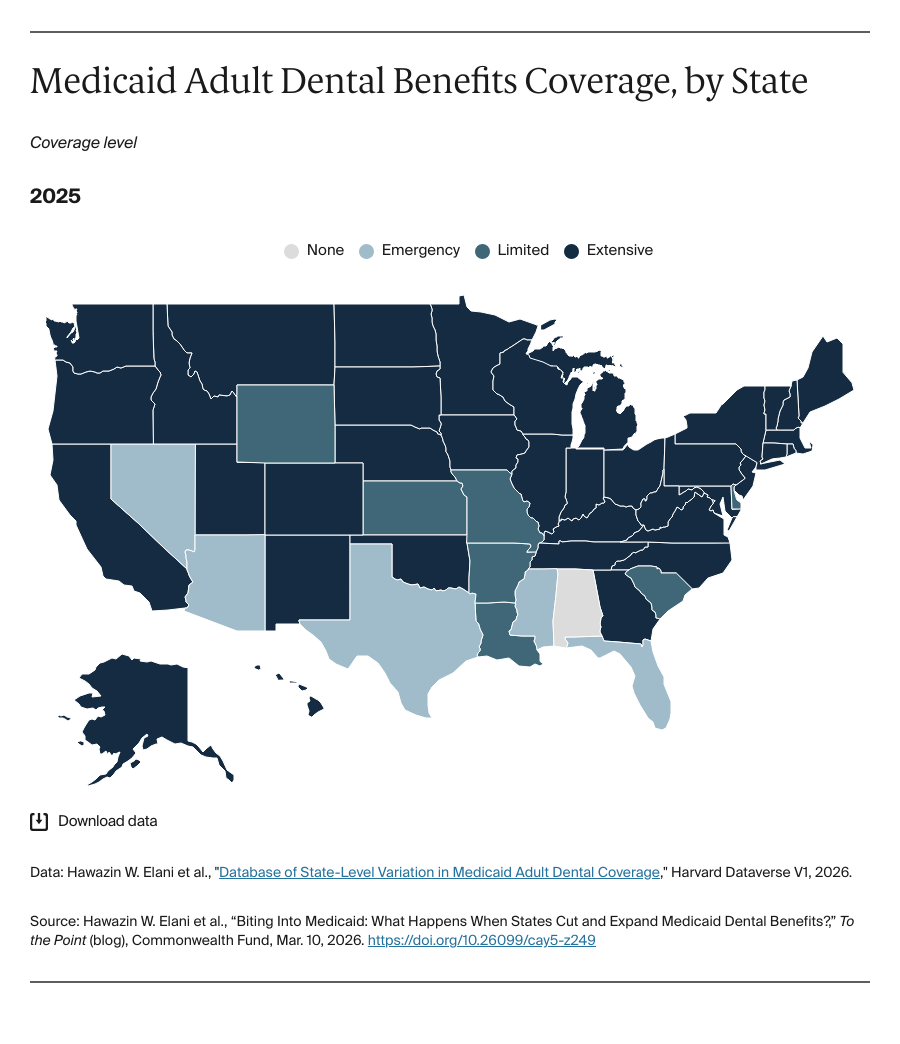
Adult dental coverage may once again be the focus of cost-cutting proposals as state legislatures debate strategies to balance budgets following the passage of the federal tax and spending law, H.R. 1.
Dental health is essential to overall well-being, helping prevent serious diseases, reducing the risk of complications from chronic conditions, and supporting nutrition and function as people age. But because adult dental coverage is optional under Medicaid, states have expanded or eliminated this benefit in response to fiscal conditions. This is concerning, since low-income enrollees are three times more likely than higher-income adults to have untreated dental infections, and twice as likely to have gum disease and unmet dental needs due to cost.
In a new Health Affairs analysis, we studied low-income adults ages 50 to 64 using Health and Retirement Study data from 2010 to 2021. We created a comprehensive database of state Medicaid adult dental benefits over time, then compared what happened after states eliminated adult dental benefits versus what happened when they expanded them.
We found that losing adult dental benefits was associated with larger and more persistent declines in dental visits than the gains observed when benefits were added. In addition, many beneficiaries were unaware of changes in dental coverage.
These findings offer a clear caution: cutting adult dental coverage can produce large and long-lasting reductions in access, while restoring coverage later may not fully undo those effects.