Introduction
Why Measure Health Disparities?
Disparities in health and health care between racial and ethnic groups do not exist in the abstract. In every U.S. state, differences in access to care, quality of care, or outcomes of care affect people’s health and well-being: whether they can afford to see a doctor or fill a prescription; whether a preventable or treatable condition like hypertension or diabetes is diagnosed and treated early; whether an illness undermines a family’s financial stability; or whether people trust the health care system enough to seek care when they need it.
By measuring and reporting on health disparities, we help to ensure that people’s health care experiences and outcomes are not hidden in averages for the entire population. Having this information enables states and health systems to assess how well they are using resources to improve health outcomes for everyone. As this report shows, state policy choices can either reduce disparities or allow them to widen, with lasting consequences for people’s health.
Since 2021, the Commonwealth Fund has published two reports examining health disparities between racial and ethnic groups across the United States and tracking differences within and between states. We’ve focused on three core areas of health system performance: access to affordable care, quality and use of health services, and health outcomes. In this third edition of the State Health Disparities Report, we draw on the most recent nationally comparable data available (2022–2024) to evaluate these differences. (For more complete details on our methods, see How We Measure Performance of States’ Health Care Systems for Racial and Ethnic Groups.)
What’s Changed Since Our Last Report
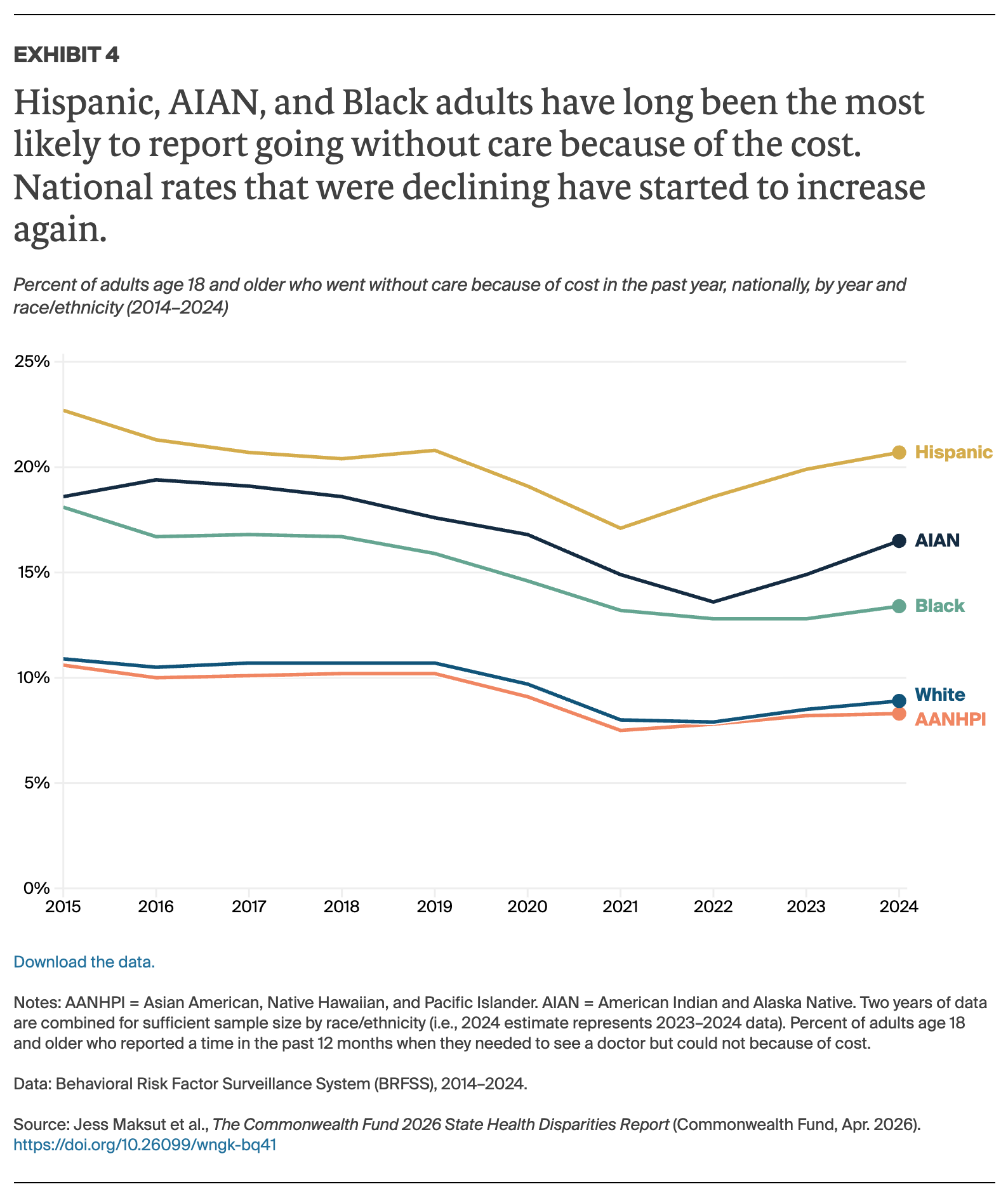
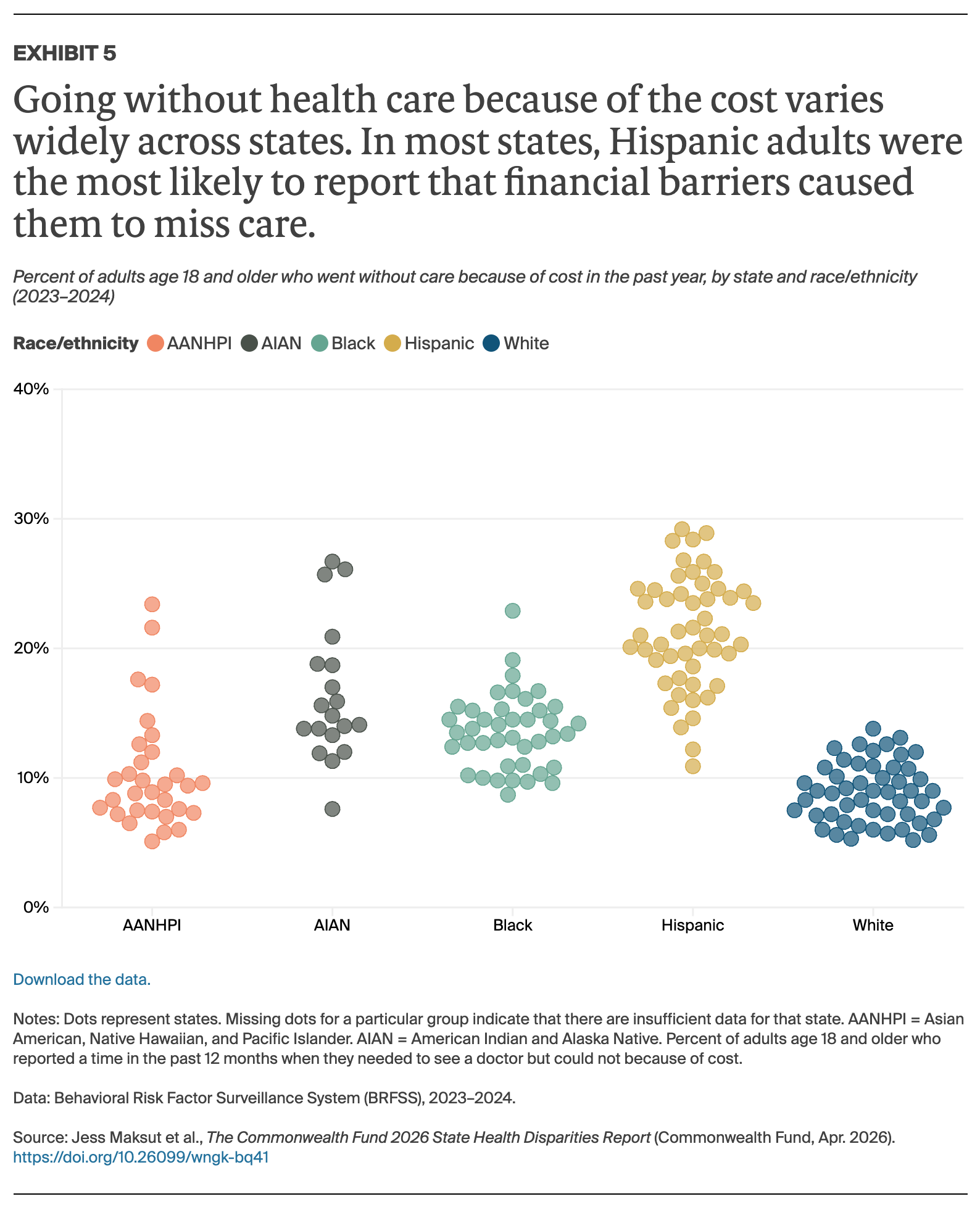
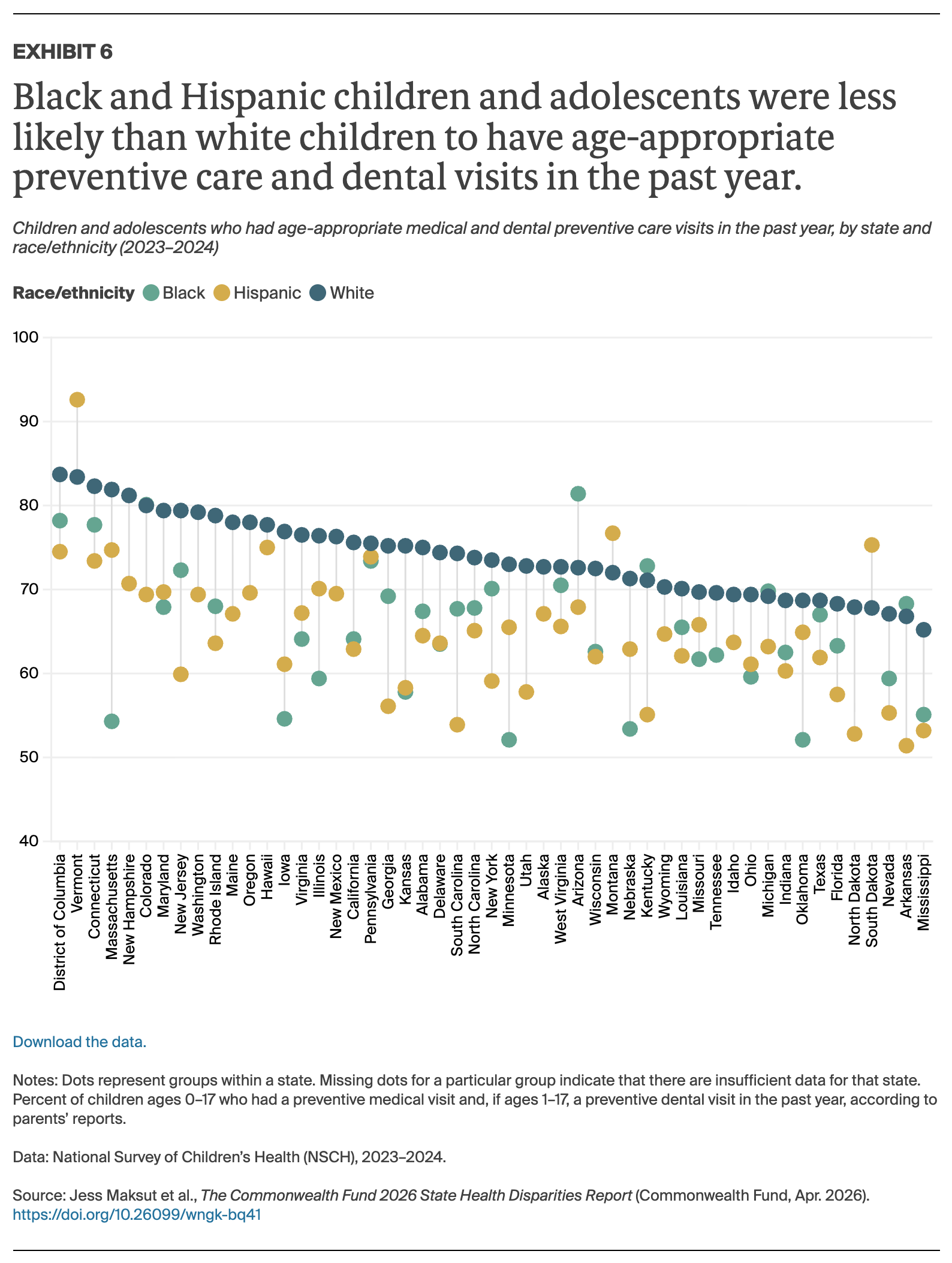
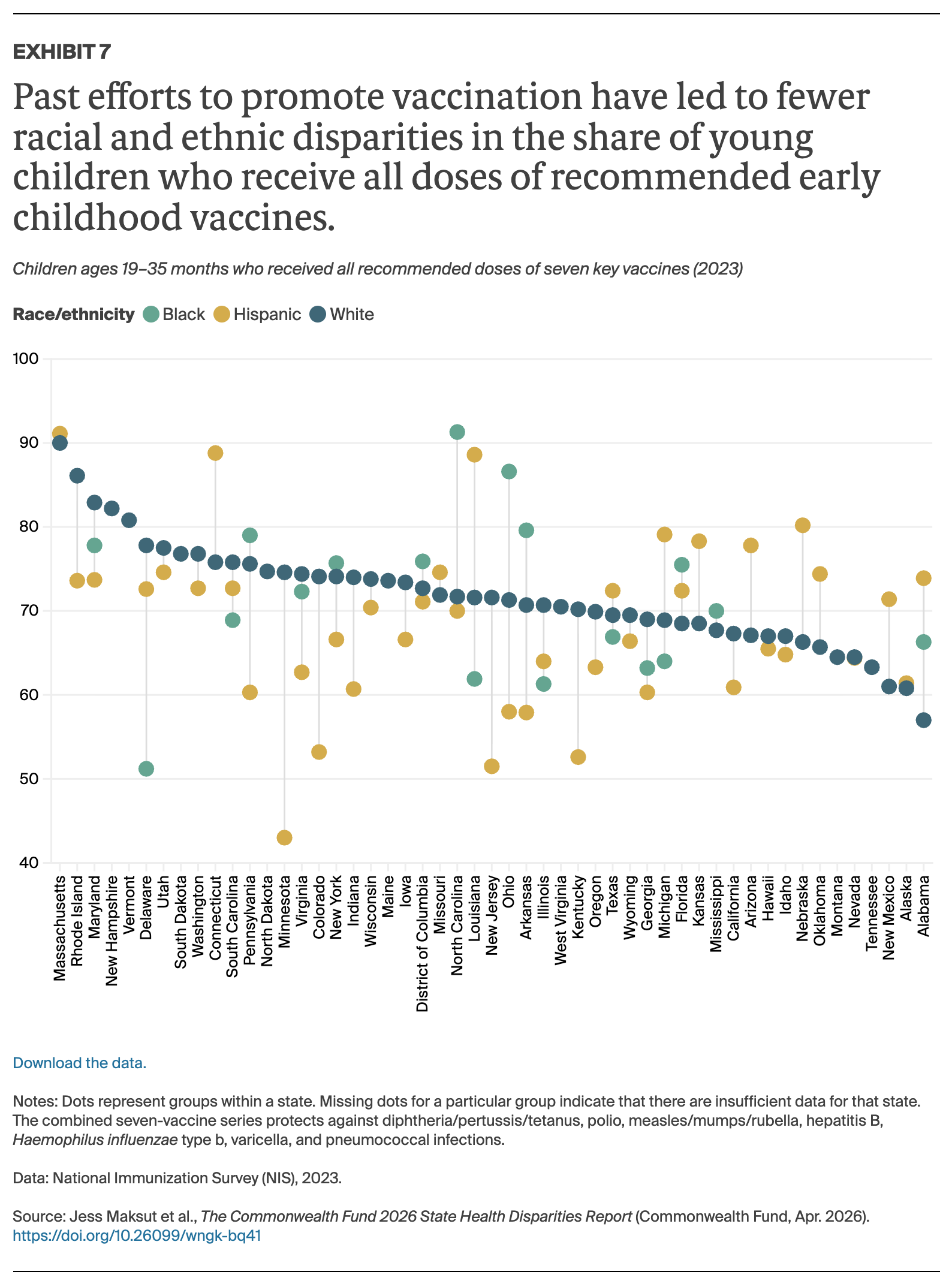
Overall, our findings show that health care in the United States continues to be unequally distributed, with racial and ethnic disparities in insurance coverage and access to high-quality care contributing to shorter, sicker lives for millions of Americans.1 As in earlier editions, we found that no state has eliminated these disparities, and sometimes stark differences persist between racial and ethnic groups.2
The period that this report covers, 2022 to 2024, saw significant gains in health coverage. North Carolina and South Dakota both expanded eligibility for Medicaid, as the majority of other states had already done; enrollment in Affordable Care Act (ACA) marketplace plans occurred at a record pace; and many state Medicaid programs extended postpartum coverage for mothers to one year.3
At the same time, there was a rollback of Medicaid coverage flexibilities adopted during the COVID-19 pandemic, and the policy of continuous Medicaid enrollment ended. These changes led to millions of Americans losing their coverage or experiencing new barriers to enrollment, effects borne disproportionately by Black and Hispanic people.4
Though not reflected in this report’s findings (owing to a lack of more current data), pronounced shifts in the national policy environment in 2025 and 2026 have likely worsened — and are on track to further exacerbate — existing racial and ethnic disparities in access, affordability, and outcomes. These include major federal funding cuts and changes to Medicaid and the ACA marketplaces; bans on eligibility for most legal immigrants and asylees; sweeping new regulations that are likely to reduce marketplace plan enrollment and increase patients’ out-of-pocket costs; and the expiration of enhanced premium tax credits, which had doubled enrollment in marketplace coverage.5
In addition, the Trump administration’s heightened immigration enforcement has caused many people, including citizens and those with lawful documentation, to avoid seeking care or participating in benefits for which they’re eligible.6 Many federal offices, positions, programs, and grants designed to advance health equity have also been eliminated.7 In this context, our findings highlight just how consequential states’ policy choices will be to people’s health in the years ahead.
Why Do We Focus on Race and Ethnicity?
While health disparities — differences in health outcomes, coverage, and quality of care — are also based on income, geography, and other factors, in this report we focus on race and ethnicity. That’s because racial disparities are among the most persistent and well documented in the U.S. health care system.8 Landmark studies have shown that racial and ethnic disparities remain even after accounting for insurance coverage, income level, and access to care. The root causes for these disparities are multifactorial, and include the historical and continued consequences of structural racism,9 the impact of social drivers of health, variations in health coverage, and unequal treatment within health care.10
The significant variation in states’ progress on health disparities is shaped by policy choices and health system investments in strategies known to improve access, quality, and outcomes for all people. In the findings that follow, the impact of state actions becomes clear.