Background and History
Over the decades, several government-funded health insurance programs have been introduced to improve coverage for specific populations, with variations across India’s 28 states and eight union territories. The Employees’ State Insurance Scheme (Karmachari Rajya Bima Yojana), launched in 1948, provided medical care and cash benefits to factory and wage-earning workers engaged in industrial labor. This was followed by the Central Government Health Scheme in 1954, offering comprehensive health care to government employees and their families.
Private-sector involvement in health coverage started in 1986 with the General Insurance Corporation of India’s Mediclaim policy, which introduced voluntary insurance for hospitalization expenses up to a defined annual limit while excluding categories such as maternity care and preexisting health conditions. The sector was still heavily dominated by state-owned monopolies until 1994, when it was liberalized by the government. In 1999, the Insurance Regulatory and Development Authority of India was established to regulate the entire insurance sector and enable the participation of private health insurers.
Initiatives to provide financial protection for unorganized workers lacking social security or health benefits and for people below the poverty line have included the National Illness Assistance Fund (Rashtriya Arogya Nidhi, 1997), Jeevandayee Yojana, the Universal Health Insurance Scheme (2003), and National Health Insurance Programme (Rashtriya Swasthya Bima Yojana [RSBY], 2008).
In 2018, the central government approved the implementation of Ayushman Bharat Pradhan Mantri Jan Arogya Yojana (AB PM-JAY), which was positioned as a significant step toward achieving universal coverage. However, the program’s efficacy has been questioned: a study one year after its launch found that insured individuals had similar rates of out-of-pocket spending as uninsured individuals.
The Role of Public Health Insurance
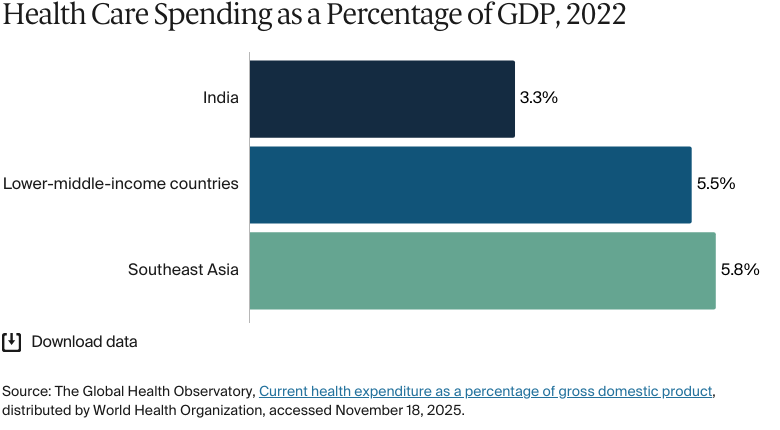
Public spending accounted for 48 percent of total health expenditure as of 2022.
AB PM-JAY is the flagship public health insurance program. Previously known as the National Health Protection Scheme, it provides INR 500,000 (USD 5,975) per family per year for secondary and tertiary care hospitalizations. Covering the bottom 40 percent of the population — about 120 million poor and marginalized families, or some 550 million total beneficiaries — it’s the world’s largest health insurance program. A significant recent expansion under AB PM-JAY that extends health coverage to all adults age 70 and over, irrespective of income, was announced in 2024. AB PM-JAY is entirely government-funded, with costs shared between the central and state governments.
AB PM-JAY subsumed RSBY in 2018, an earlier government-funded insurance initiative aimed at families below the poverty line, with a family cap of five members. RSBY provided coverage of up to INR 30,000 (USD 359) per family per year for inpatient hospitalization expenses but did not include outpatient care.
Despite its limited scope, RSBY played a foundational role in shaping India’s approach to public health insurance for the informal sector. One example is the Central Government Health Scheme, which is operated by the Ministry of Health and Family Welfare (MoHFW, Swāsthya Aur Parivār Kalyān Mantrālaya) to cover current and retired central government employees and their dependents. Coverage includes homeopathic and alternative medicine treatments. It’s a subscription-based model where beneficiaries contribute a fixed monthly rate that ranges from INR 250 (USD 3) to INR 1,000 (USD 12) based on salary. About 4.6 million beneficiaries have been registered under the program.
The Common Man Insurance Scheme (Aam Aadmi Bima Yojana) is a government social security program that provides death and disability coverage. It covers one earning member (ages 18 to 59) per family, with an annual premium of INR 200 (USD 2.4) per person, shared equally by the central and state governments.
The only health insurance program that both employees and employers contribute to is the Employees’ State Insurance Scheme, run by the Ministry of Labour and Employment for companies with 10 or more workers. Employees contribute 0.75 percent of their wages, and employers contribute 3.25 percent. To be eligible, a worker must earn up to INR 21,000 (USD 251) per month. Coverage for workers and their families includes maternity care and disability and death benefits for employment-related injuries. State governments contribute one-eighth of the medical benefit expenditures, up to an annual per capita ceiling of INR 1,500 (USD 18). As of 2024, the program had about 144 million beneficiaries.
Many Indian states run their own health insurance programs to address regional needs. For example, Maharashtra operates the Mahatma Jyotiba Phule Jan Arogya Yojana, Tamil Nadu offers the Chief Minister's Comprehensive Health Insurance Scheme, and Andhra Pradesh runs the Dr. YSR Aarogyasri Health Insurance Scheme, launched to support low-income families.
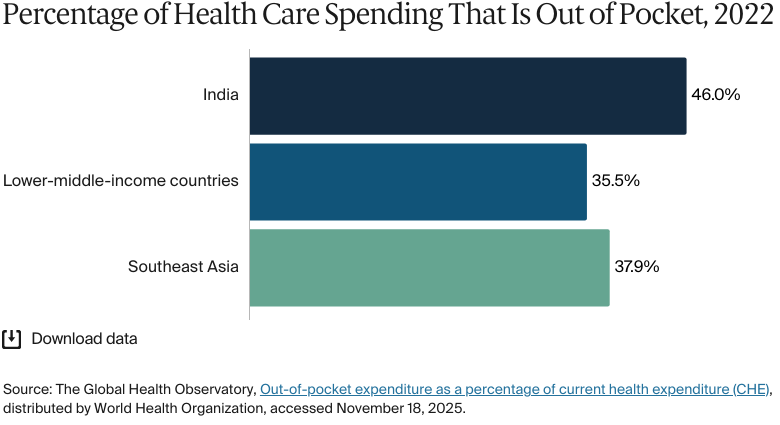
Despite government initiatives such as AB PM-JAY, about 30 percent of Indians remain uninsured. This gap stems mainly from outdated eligibility data, low awareness among eligible families, and fragmented state-level program implementation. Even among those covered, underinsurance persists, as coverage limits often fall short of actual treatment costs, leaving many exposed to significant out-of-pocket spending.
Services Covered by Public Health Insurance
The following services are covered by public health insurance:
- Preventive care
- Inpatient care
- Outpatient care
- Maternity care
- Primary care
- Pharmaceuticals
- Dental care
- Eye care
- Mental health care
- Palliative care
- Long-term care
- Rehabilitative care.
Safety Nets
India’s various health coverage programs subsidize care for different populations. AB PM-JAY is the largest among them. The core principle of the program is to eliminate user charges at the point of service, as the government directly reimburses empaneled hospitals. However, implementation of this policy, particularly in the private sector, has often been inconsistent. While the program is promoted as providing fully free care, many patients end up paying out of pocket when package limits are exceeded.
In addition to AB PM-JAY, other government initiatives aim to shield beneficiaries from user charges. For instance, the Employees’ State Insurance Scheme for workers in the organized sector and the Central Government Health Scheme for central government employees both offer subsidized care with no upfront payments.
To help make medicines affordable, the Pradhan Mantri Bhartiya Janaushadhi Pariyojana (PMBJP) ensures access to essential generic drugs at lower prices. Several states also operate their own health insurance programs. Notably, Tamil Nadu and Andhra Pradesh were among the first to launch large-scale programs, providing inpatient coverage for low- and even some middle-income populations.
Limited financial protection is a barrier to equitable health care. With minimal risk-pooling, households often face high out-of-pocket costs. Some programs, including the Employees’ State Insurance Scheme, exempt low earners (earning up to INR 176/USD 2 per day) from contributions. However, these safeguards aren't a feature of every program.
The Role of Private Health Insurance
The Insurance Regulatory and Development Authority Act of 1999 allowed private companies to enter the health insurance market. It also allowed individuals who aren’t eligible for sponsored insurance programs to purchase a private policy.
Since 2020, the Insurance Regulatory and Development Authority of India required employers operating during the COVID-19 lockdown to provide group health insurance to their employees, a measure that has since encouraged wider adoption of employer-sponsored health coverage.
People are increasingly turning to personal private health insurance plans to supplement their employer-provided coverage, signaling a growing demand for more comprehensive and customizable protection. As of 2022, private insurance accounted for 7.4 percent of total health expenditures.
The Role of Government
Responsibility for the governance, financing, and operation of the health system is divided between the central and state governments. At the federal level, the MoHFW has regulatory power over most health policy decisions, although the ministry isn’t directly involved in health care delivery. It comprises two departments:
- The Department of Health and Family Welfare, which is responsible for organizing and delivering all national health programs, with each program headed by its own administrative body.
- The Department of Health Research, which is responsible for health promotion and clinical research, the development of health research and ethics guidelines, outbreak investigations, and the provision of advanced research training and grants for such training.
The Directorate General of Health Services, under the MoHFW, provides technical guidance on public health and medical education. It oversees national health programs and central hospitals and supports states and union territories (territories directly governed by the central government) in enhancing public health services.
At the state level, the Directorate General of Health Services and the Department of Health and Family Welfare are responsible for organizing and delivering all health care services, from primary care and pharmaceutical services to secondary and tertiary hospital care.
States are independently responsible for health care activities, so there’s significant nationwide variation in service delivery models, insurance coverage, availability, and access. Certain initiatives, such as the National Health Mission are governed or financed jointly by the central and state governments.
At the district level, local government (Panchayati Raj) institutions are responsible for grassroots governance and administration in rural villages. These government bodies play a significant role in establishing primary health centers and contributing to social policies related to education, agriculture, and transportation. The chief medical and health officer of each district is primarily responsible for the implementation of health and welfare programs at the district level.
Service provision by Panchayati Raj institutions is uneven. Residential segregation, shaped by caste and religion, strongly influences distribution. Areas dominated by marginalized groups, such as Scheduled Castes and Muslims, often receive poorer infrastructure and weaker service delivery than majority communities.
All programs under the National Health Mission are organized on a local level through District Health Missions in rural areas or City Health Missions in urban centers. These initiatives are headed up by the chairperson of the district council or the city mayor.
The National Health Authority implements national health initiatives, most notably AB PM-JAY.
Integration and Care Coordination
Patient care in India is fragmented. Although a patient referral mechanism exists, it’s rarely utilized, owing to a lack of coordination across health care levels, a lack of awareness among patients about the referral process, and limited trust in primary or secondary facilities. Many bypass the system and head straight to tertiary hospitals, overloading them. Meanwhile, rural and low-income populations continue to struggle with communication gaps associated with language differences and illiteracy, under-resourced primary care, affordability issues, and geographic barriers. This worsens health care inequities (See Addressing Health Inequities).
The National Health Authority is working to improve care coordination by integrating the Central Government Health Scheme, AB PM-JAY, the Employees’ State Insurance Scheme, and other public programs under a unified digital platform. This allows real-time updates on patients and cross-utilization of hospitals between programs. For example, AB PM-JAY beneficiaries can access Employee’s State Insurance hospitals, and vice versa, and reimbursements are based on eligibility and are at AB PM-JAY rates.
Cancer care is provided under a hub-and-spoke model that improves integration and coordination by linking primary care centers (spokes) with specialized tertiary hospitals (hubs). It’s a patient-centric approach that speeds up referrals and streamlines follow-up appointments.
Overview of the Delivery System
The health care delivery system operates through a three-tiered structure:
- Primary care. Preventive, curative, and maternal services are offered in primary health centers and community health centers. These facilities are patients’ first point of contact with the health system.
- Secondary care. Primary and community health centers refer patients with complex health conditions to subdistrict and district hospitals for specialized diagnostics, surgeries, and inpatient care.
- Tertiary care. Highly specialized health care for complex conditions is provided by advanced facilities, such as medical colleges and specialty hospitals.
Coverage programs, such as the Central Government Health Scheme and AB PM-JAY, provide free treatment: beneficiaries can obtain care at participating facilities by using digitally enabled identification cards or smart cards. Under AB PM-JAY, beneficiaries get an Ayushman card to access services at any public or private empaneled hospital (one recognized and approved by an insurance company or government program).
Provider payments made by AB PM-JAY follow a case-based bundled pricing model in which health care providers are reimbursed at a fixed rate for a defined set of services under specific health benefit packages. To increase efficiency and care quality, the program is transitioning to a diagnosis-related, group-based payment system, which considers case severity.
Primary Care
By July 2025, 178,154 Ayushman Bharat health and wellness centers had been established. These are also known as Ayushman Arogya Mandirs (AAMs). The centers provide comprehensive primary health care — including preventive, promotive, curative, rehabilitative, and palliative services — free of charge to all age groups.
Residents aren’t required to register with a general practitioner (GP), as the concept of GPs does not formally exist within the public health system. Primary care is provided by a network of government health facilities and community health workers or mid-level health care providers. Primary health care was originally structured as a three-tiered system — sub-health centers, primary health centers, and community health centers — each serving different population sizes with specific services. Each primary health center provides curative and preventive services to between 20,000 and 30,000 people. Sub-health centers, the first point of contact for patients, are designed to handle maternal and child health, disease control, and health counseling for a population of 3,000 to 5,000. Initially upgraded to health and wellness centers in 2018, these facilities have now been further enhanced and rebranded as AAMs for broader and improved primary health care services.
All medical personnel working at public outpatient or inpatient facilities, including primary and specialty physicians, are paid salaries, which vary based on the area of work and level of specialization. However, several state governments are enhancing service delivery by introducing performance-based payments for Accredited Social Health Activists. Studies highlight that well-designed performance-based payments that follow clear guidelines and are made electronically have strengthened the performance of health workers. In addition to the fixed monthly incentive of INR 2,000 (USD 24), a number of states have proposed increasing payments based on performance.
Physicians are generally prohibited from engaging in private practice during their official hours. However, the enforcement and specifics of this rule vary by state.
Traditionally, primary health centers operated during standard daytime hours. However, recent initiatives aim to enhance accessibility by converting primary health centers into 24/7 facilities. As of 2023, more than 12,000 primary health centers have been upgraded to provide around-the-clock services, particularly to improve emergency care in rural and underserved regions.
There are no data available on the number of GPs in the country.
Outpatient/Specialist Care
Community health centers also provide outpatient specialist care delivered by surgeons, obstetricians, pediatricians, and anesthesiologists, among others, as well as necessary infrastructure, such as an operating theater and a blood storage unit. Each center covers between 80,000 and 120,000 people.
All outpatient specialized services not provided at community health centers are referred to district hospitals. The government plans to establish day care cancer centers in all district hospitals over the next three years, targeting 200 centers in fiscal year 2025–26 to enhance access to cancer care at the district level.
First referral units (FRUs) are upgraded community health centers equipped to provide comprehensive emergency obstetric and newborn care, including cesarean sections, emergency treatment for sick children, and referral transport. The number of operational FRUs increased from 940 in 2005 to more than 3,000 in 2024. In urban areas, community health centers serve as FRUs by default.
In outpatient care, 64 percent of patients sought treatment from private facilities in 2022, whereas only 22.8 percent accessed services through public health care institutions.
Physician Education and the Workforce
Medical education is provided by both government-led institutions and private colleges. The fee structure for an undergraduate medical degree depends on whether it's a government or private college. Government institutions offer more affordable education, with annual fees typically ranging from INR 75,000 to 220,000 (USD 896 to 2,629) in 2024, compared with INR 400,000 to INR 4 million (USD 4,780 to 47,803) at private colleges.
The National Medical Commission sets medical education standards, accredits programs, recognizes foreign degrees, and maintains a national physician register. It also has a remit to improve access to affordable quality medical education, work toward equitable workforce distribution, and promote universal health care.
Between 2019 and 2025, the number of medical colleges rose from about 500 to nearly 800. However, physician migration is high: more than 2,800 doctors left the country in 2021 alone.
There are no data available for the number of medical graduates in the country.
Hospitals