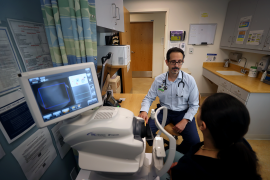
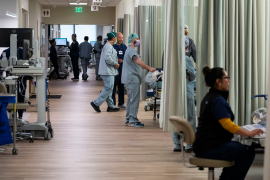
The COVID pandemic accelerated the adoption of telemedicine, with Medicare and other insurers expanding coverage of the service. However, there has been ongoing debate about how much insurers should pay for virtual visits — or if they should pay at all. The patients and clinicians who use these visits find them to be a convenient complement to in-person care that work well in many clinical scenarios, while policymakers have wondered how virtual visits impact care quality and spending.
One question centers on virtual visits and the use of low-value care — that is, medical tests and other services such as Pap smears and prostate cancer screenings in older adults that offer little to no benefit yet can cause direct or cascading harms. Telemedicine may reduce low-value testing by creating barriers to completing these tests at a given visit. Alternatively, it could increase low-value testing by lowering the bar to having a visit in the first place or if clinicians order tests to search for information or reassure patients in the absence of a physical exam. Prior evidence was mixed and largely limited to studies of direct-to-consumer telemedicine companies rather than looking at virtual visits as part of usual care.
To get at these questions, our research team first used a quasi-experimental difference-in-differences approach that took advantage of natural variation in health systems’ telemedicine adoption. Specifically, we analyzed 2019–2022 national claims data for more than 2 million traditional Medicare beneficiaries who received their care (since before the pandemic) in health systems across the United States that either did or did not adopt telemedicine at high rates during the pandemic. Compared to patients in low-adoption telemedicine systems, those in high-adoption telemedicine systems had slightly higher rates of total visits (0.12 additional visits per person-year, including virtual or in-person). They also had lower use of seven of the 20 low-value tests we studied (with individual testing rates declining by up to 2 percentage points relative to nonadopting systems), particularly for tests like cervical cancer screenings and blood tests that are usually offered at point of care. Patients in high-adoption telemedicine systems had $48 lower spending per-person on visits each year, likely because of lower intensity billing for virtual visits. They also had either similar or lower spending on each of the low-value tests. In short, our analysis, consistent with another claims study of Michigan primary care practices, found that virtual care is associated with less low-value testing, even while contributing to a small rise in visits that may offer more testing opportunities.
Next, we examined the patient and clinician behaviors underlying these results. Using 2022–2024 electronic health record data from Mass General Brigham’s multistate health system, we matched virtual and in-person annual visits to compare patterns of test ordering by clinicians and completion by patients. We found that both high-value and low-value tests were less likely to be ordered and completed in virtual (vs. in-person) visits, with larger drops for low-value tests than for high-value tests. We also found that point-of-care laboratory tests like diabetes screening tests and urinalyses saw larger drops in ordering and completion than scheduled tests, like colorectal cancer screenings and mammography. In other words, telemedicine seemed to introduce friction for both clinicians and patients that may differentially reduce low-value testing, especially for tests offered at point-of-care.
Medicare telemedicine coverage has been temporarily extended again, through the end of 2027. Our results, taken together with other mixed results on telemedicine’s impact on spending and quality, provide some reassurance to policymakers that telemedicine coverage has not resulted in increased testing or spending and may, in some cases, encourage patients and clinicians to make more careful use of point-of-care medical tests. Our finding that telemedicine may also impede high-value testing, however, cannot be overlooked. It is possible that high-value tests not ordered during virtual annual visits are addressed at other points in the year. Past research that found no link between health system telemedicine adoption and high-value screening rates lend credence to this idea, but the declines highlight the importance of tools like gap closure alerts and population health registries. With careful design, health systems and policymakers can harness telemedicine to reduce patient burdens and avoid the cascading harms of low-value testing while still ensuring access to high-value services.