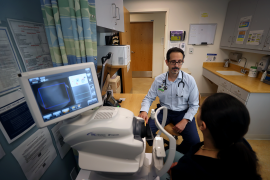
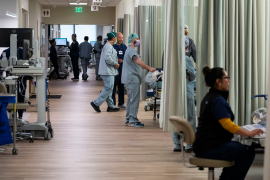
H.R. 1 made deep cuts to Medicaid and the Supplemental Nutrition Assistance Program but also established the Rural Health Transformation Program (RHTP), which will provide $50 billion over five years to all 50 states with the goal of strengthening rural communities by transforming the rural health care delivery system.
States will all be crafting their own plans and awarded different amounts, so there will be a range in terms of implementation, effectiveness, and impact. It’s important to monitor these plans to assess effectiveness and to discover the programs, methods, and system changes that are leading to success.
Can the RHTP Be Transformational?
One of the RHTP’s goals is to transform rural health care systems — not just in terms of delivery, but the payment, workforce, and information systems that shape them. But transformation can be difficult to achieve and hard to measure. Because the RHTP is structured around annual renewals and has guardrails about what states can and cannot do with the funds, states will be limited in their ability to implement changes that require a longer outlook. If states cannot demonstrate success in a short period, they risk a reduction in future funding, which could have a dampening effect on transformation. While the Centers for Medicare and Medicaid Services has made assurances that progress toward program implementation and keeping to the proposed timeline will be used to assess success, there may be hesitancy about making long-term changes.
All state plans have been submitted; several proposed fixes to the inadequate volume-based payment system that is particularly unsuitable for rural care delivery. Truly transformative payment reform for rural health care would require time, innovation, and multiple payments methodologies. These have been proposed in some state plans, offering a combination of capacity support and value-based purchasing. Alaska will use different payment strategies to move rural providers away from relying on volume-based reimbursement and into a more financially stable model. South Dakota proposes to introduce capitated payment for rural primary care — that is, upfront predictable payments that can improve care delivery and financial sustainability for practices.
Transformational care also relies on robust networks of coordinated care that connect local clinical care, social services, and other health-related services to regional services. This “hub-and-spoke” care model — which is being proposed in Florida and California — would require coordination among organizations, information sharing, and other resources for patients.
To address workforce shortages, states have proposed pipeline development, incentive programs, rural training programs, and loan repayment. Without truly transformational change in medical education, student debt, and ongoing payment, recruitment and retention will remain a patchwork of temporary fixes. Real transformation would require low- or no-cost training for rural providers, stable funding for rural primary care, tax breaks and other long-term financial incentives, scope-of-work reforms, and greater use of allied health professionals and team-based care. Delaware is proposing a new medical school in conjunction with scholarships for rural providers to eliminate debt burdens.
The proposals also include initiatives aimed at improving data sharing and advanced informatics. These programs range from building interfaces for electronic health records across systems in Hawaii and Rhode Island, aggregated data analytics in Idaho and South Dakota, and increasing the use of artificial intelligence in Maine and Utah. These changes would allow for greater use of telehealth, remote patient monitoring, and information sharing.
Will the Money Go to Rural Communities and Health Care Systems?
A key metric of success should be how much money flows to rural communities, providers, hospitals, and facilities. Rural providers are financially vulnerable and constantly battling to care for their communities on razor-thin — sometimes negative — operating margins. States should ensure that funds flow to rural providers and not only to urban systems that promise to increase services in rural areas. One way to do this is to create coordinated regional networks, by directly funding rural organizations, to improve care coordination when rural patients seek care elsewhere. This approach is vital for long-term success of the RHTP.
Considering the emphasis on technology, there are concerns funding could go to external vendors. Iowa and Delaware have proposed creating “technology catalyst funds” to increase the integration of tech-enabled care in rural communities. It is unclear if such organizations will be closely tied to rural communities or if states will need to secure commitments prior to awarding funds. Without this connection, it is possible that programs — and revenues — won’t be centered in the communities. If these external groups supplant, rather than supplement, local in-person care with distant options, they could further weaken rural systems. Many of these innovations are expensive to obtain and maintain. While RHTP funds would facilitate adoption, ongoing, sustainable funding would be difficult without system integration.
Will RHTP Create Institutional Change?
There is wide variation in the level of institutional changes being proposed, with some states taking a centralized approach by establishing divisions to manage their programs in rural health. New Hampshire, for example, is creating a Governor’s Office of New Opportunities and Rural Transformational Health that reports to the governor. The office will coordinate the RHTP and be part of the governance structure for the foreseeable future.
Other states are hiring RHTP directors and staff to manage the program, but as part of existing divisions and entities. These proposals will implement programs either directly from these existing organizational structures or in collaboration with external partners. Virginia and North Carlina are taking this approach and are in the process of hiring RHTP directors.
Other states are taking a combined approach — identifying specific programs they will manage while also funding external programs and partners. Still others, like South Carolina, are taking a decentralized approach, by proposing to distribute much of the funds to external collaborators, vendors, and consultants.
Conclusion
The Rural Health Transformation Program presents an opportunity for rural delivery systems to transform, enhance care, and improve outcomes for their communities. Ultimately, success will hinge on the level of transformation, integration, and local funding that occurs in the next five years. Rural communities are resilient, creative, and effective at caring for their communities with limited resources; we can all learn from these innovative models of care.