The COVID-19 pandemic has wreaked havoc on the U.S. economy and put countless businesses at risk of failure. The health care industry has been hit particularly hard because of drops in revenue driven by decreases in elective care, stay-at-home orders, and the costs of preparing for a pandemic, such as increasing hospital capacity and purchasing personal protective equipment. Recognizing these challenges, and the critical role the industry plays, Congress and the U.S. Department of Health and Human Services (HHS) acted quickly to support the health care system and frontline workers in three primary ways: provider relief funds, the Paycheck Protection Program, and the Medicare Accelerated and Advance Payment Program.
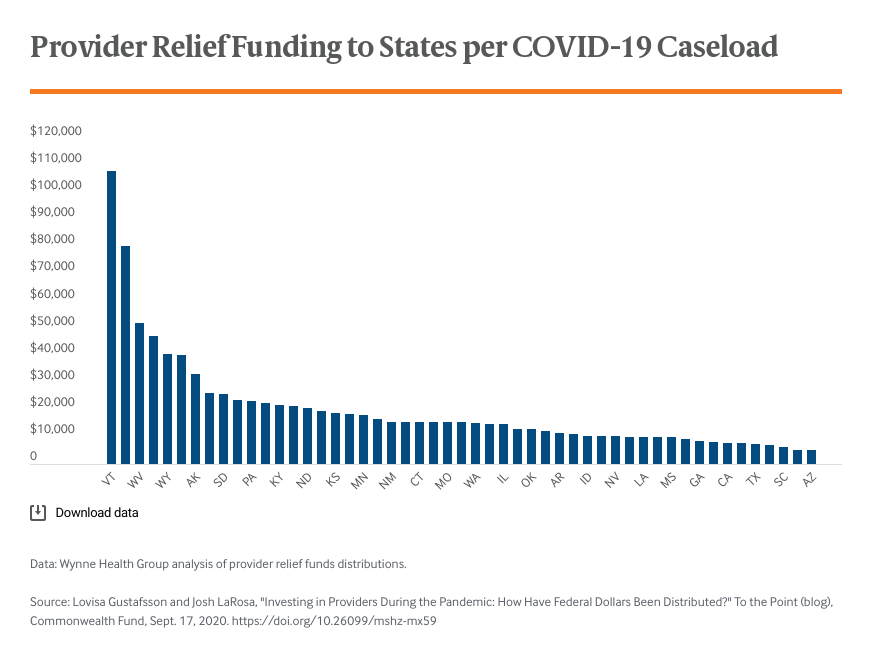
The support was intended to compensate providers for drops in revenue, shore up provider finances during the disruption, and preserve jobs. Lawmakers also recognized the importance of supporting the pandemic response itself, by: providing assistance to “hot spots,” supporting financially vulnerable providers who are least able to afford the additional costs of the pandemic, and ensuring access to COVID testing and services to the uninsured. But this wide range of goals has led to some confusion: Who should get relief funds? How much is enough?
A Closer Look at Provider Support
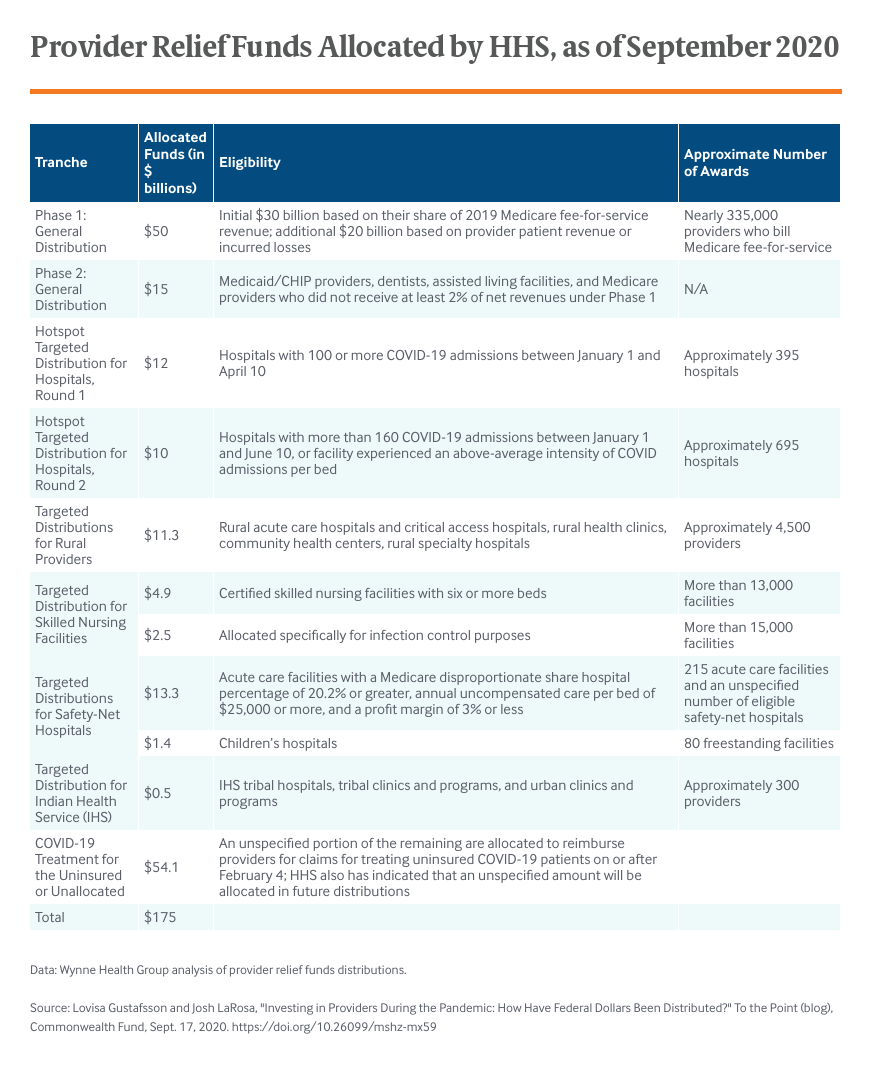
The CARES Act and Paycheck Protection Program and Health Care Enhancement Act provided the largest amount of funding for health care providers by appropriating a combined $175 billion to the provider relief funds. For context, Medicare spent $147 billion on inpatient services for all of 2019.
There was little to no guidance or established rules on how to distribute an investment of this size efficiently and effectively in a pandemic. As a result, HHS was left to determine how to best allocate these dollars.